- Home
- »
- Healthcare IT
- »
-
U.S. Medical Coding Market Size, Industry Report, 2033GVR Report cover
![U.S. Medical Coding Market Size, Share & Trends Report]()
U.S. Medical Coding Market (2026 - 2033) Size, Share & Trends Analysis Report By Classification System (ICD, HCPCS, CPT), By Component (In-house, Outsourced), By Medical Specialty (Oncology, Cardiology, Anesthesia), By End Use, And Segment Forecasts
- Report ID: GVR-3-68038-025-5
- Number of Report Pages: 90
- Format: PDF
- Historical Range: 2021 - 2025
- Forecast Period: 2026 - 2033
- Industry: Healthcare
- Report Summary
- Table of Contents
- Segmentation
- Methodology
- Download FREE Sample
-
Download Sample Report
U.S. Medical Coding Market Summary
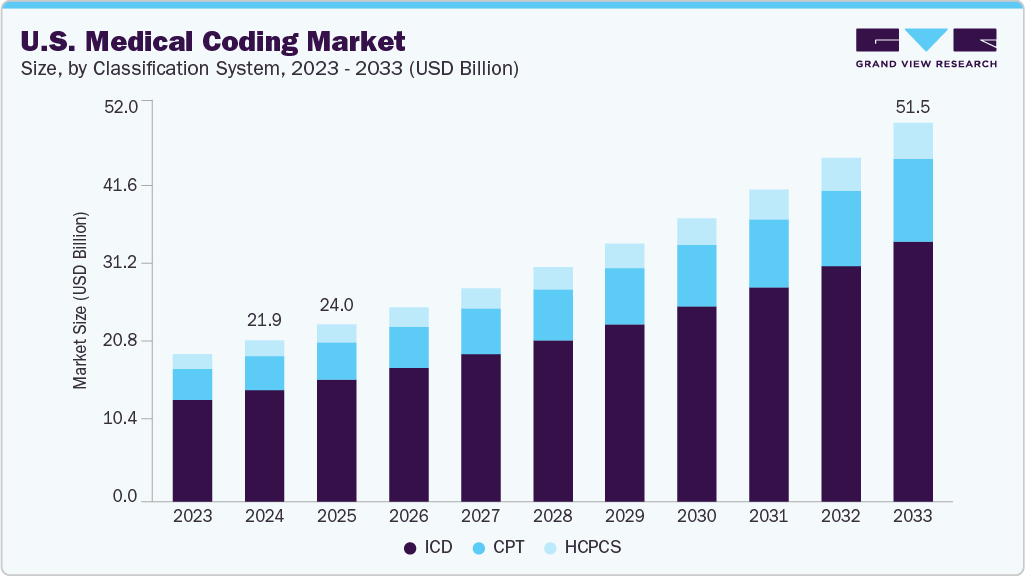
The U.S. medical coding market size was estimated at USD 21.6 billion in 2025 and is projected to reach USD 44.4 billion by 2033, growing at a CAGR of 9.6% from 2026 to 2033. Errors in billings, insurance fraud, and misinterpretations of medical documents result in large financial losses. Increasing losses due to ineffective medical billing and revenue cycle management are increasing demand for revenue cycle management including medical coding software and services. This, in turn, is estimated to drive market growth potential.
Key Market Trends & Insights
- Based on component, the outsourced segment held the largest market share of 64.8% in 2025.
- Based on classification system, the ICD code segment held the largest market share of 69.3% in 2025.
- Based on medical specialty, the anesthesia segment held the largest market share of 10.8% in 2025.
- Based on end use, the acute care hospitals segment held the largest market share of 76.9% in 2025.
Market Size & Forecast
- 2025 Market Size: USD 21.6 Billion
- 2033 Projected Market Size: USD 44.4 Billion
- CAGR (2026-2033): 9.6%
Market Drivers & Dynamics
The growing preference for outpatient healthcare delivery in the U.S. is significantly influencing the demand for medical coding services. Hospitals and health systems increasingly prioritize outpatient departments to manage rising patient volumes while improving operational efficiency. Moreover, ambulatory surgery centers (ASCs) significantly contribute to the growth of outpatient care in the U.S., providing same-day surgical procedures in specialties such as orthopedics, ophthalmology, gastroenterology, and pain management. With more than 6,000 centers nationwide performing over 20 million procedures annually, outsourcing of medical coding services is expected to rise over the forecast period.
Moreover, CMS continues to add procedures to the ASC-covered list, encouraging migration of surgical services away from inpatient hospital settings. For instance, in November 2025, CMC added 276 procedures to the ASC Covered Surgical Procedures and Ancillary Services Lists (CPL) and added an additional 271 codes to the ASC CPL.
In addition, the growing volume of healthcare administrative transactions in the U.S. is a significant driver of the medical coding market. For instance, according to the 2023 CAQH Index Report, the U.S. healthcare industry processed over 59 billion administrative transactions in 2023, including claims submissions, eligibility checks, claim status inquiries, and prior authorization requests. Among these, medical claims submission represents one of the most critical processes within healthcare revenue cycle management.
Furthermore, development of artificial intelligence (AI)-enabled medical coding is estimated to drive market growth. For instance, in April 2025, the Cleveland Clinic partnered with AKASA to deploy generative AI tools in mid-revenue-cycle operations across U.S. sites, automating medical coding from clinical documents. The AI processes 100+ documents in 1.5 minutes, boosting speed, accuracy, and prior authorizations while enhancing coder efficiency for complex cases.
Technology vendors across the country continue investing in advanced AI-driven medical coding platforms that integrate directly with electronic health record systems and revenue cycle management software. In August 2025, HGM Limited, through its U.S. subsidiary Healthcare Capital Holdings LLC (HCH), announced the acquisition of Aidéo Technologies LLC, a leader in AI-powered autonomous coding solutions. This acquisition expands HGM’s capabilities in revenue cycle management (RCM), medical coding, and healthcare analytics.
“Acquiring Aidéo Technologies is a major step towards our goal of building a comprehensive AI-driven healthcare services platform. Aidéo’s Autonomous Coding Platform, built on advanced AI, natural language processing, real-time analytics, and Large Language Models (LLM), delivers accuracy that surpasses manual and traditional CAC tools. Its HL7 interoperability ensures seamless communication with industry standard EHR systems, supporting surgical specialties, emergency departments, anesthesia, radiology, and RCM companies across the U.S.”
-Dr. Bhargav Thakkar, EVP Healthcare of HGM Limited.
Market Concentration & Characteristics
The chart below illustrates the relationship between industry concentration, characteristics, and participants. The x-axis represents the level of industry concentration, ranging from low to high. The y-axis represents various industry characteristics, including industry competition, level of partnerships & collaboration activities, degree of innovation, impact of regulations, and regional expansion. The U.S. medical coding market is fragmented, with the presence of several software and solution providers dominating the market. The degree of innovation, the level of merger & acquisition activities, and the impact of regulations on industry is high. Moreover, the product substitutes in industry is moderate.
The U.S. medical coding industry for medical coding is constantly evolving with frequent introduction of new technologies and methods. Technological advancements are expected to increase the number of platforms for medical coders, which is expected to aid in the growth of the market. In addition, big data and predictive analytics applications have expanded the healthcare value chain, particularly in drug discovery, genomic research, and clinical trials. For instance, in November 2024, Maverick Medical AI launched Maverick CodePilot, an innovative real-time medical coding solution that integrates with physicians' workflows at the point of care.

Several market players are involved in merger and acquisition activities. Through M&A activity, these companies expand their geographic reach and enhance their product and service offerings. For instance, in October 2025, R1 acquired Phare Health Ltd, a technology firm developing AI-native solutions for inpatient coding and clinical documentation improvement (CDI). The acquisition strengthens R1’s strategy to accelerate AI-driven automation across the revenue cycle and advance toward near real-time medical claims adjudication. This move is expected to intensify innovation in AI-based coding solutions, driving greater automation, efficiency, and competitive expansion within the medical coding market.
Regulations have a significant impact on the U.S. medical coding market players. Constantly changing healthcare regulations can affect the demand for medical coding services and revenue of companies in this market.
Substitutes to medical coders are difficult to find. Internal substitutes, including outsourcing of medical coding, can lead to internal competition. Companies in this industry are vertically integrated, performing all activities from R&D to aftersales services.
Classification System Insights
The ICD segment held the largest revenue share of over 69.0% in 2025. The ICD classification system is a key part of the U.S. medical coding framework, standardizing documentation of diseases and related health issues across healthcare settings. According to an article published in HCPLive in February 2026, the expanded ICD-10 code structure helps clinicians and researchers better identify patient populations and capture disease-specific clinical characteristics in healthcare databases. This specificity improves epidemiological tracking, resource allocation, and reimbursement accuracy.
The CPT segment is anticipated to grow at the fastest CAGR during the forecast period. Demand for CPT coding services in the U.S. continues to increase due to rising procedure volumes, expanding outpatient care, and evolving reimbursement models. Integration of CPT coding with electronic health records and revenue cycle management platforms improves documentation accuracy and operational efficiency. Computer-assisted coding technologies are also being deployed to analyze clinical notes and suggest appropriate procedural codes. These advancements support coding accuracy while reducing administrative workload across healthcare organizations.
Medical Speciality Insights
The anesthesia segment dominated the U.S. medical coding industry, accounting for the largest share 10.8% in 2025. Accurate coding is essential for reimbursement, as anesthesia billing depends on multiple factors such as procedure type, duration, and patient condition. The complexity of anesthesia coding, including the use of time units and modifiers, drives demand for specialized coders. Hospitals and ambulatory surgery centers rely on accurate documentation to prevent claim denials. This growing procedural volume and complexity support significant segment expansion.
The cardiology segment is expected to witness growth at the fastest CAGR during the forecast period. Cardiology-related costly treatment procedures require medical coding services, as it improves the effectiveness of these procedures and helps manage medical billing, patient care, & other workflows, particularly when patients are among largest group of payers. With rising prevalence of cardiological diseases, workload on payers and hospital staff increases, thereby propelling the segment growth.
Component Insights
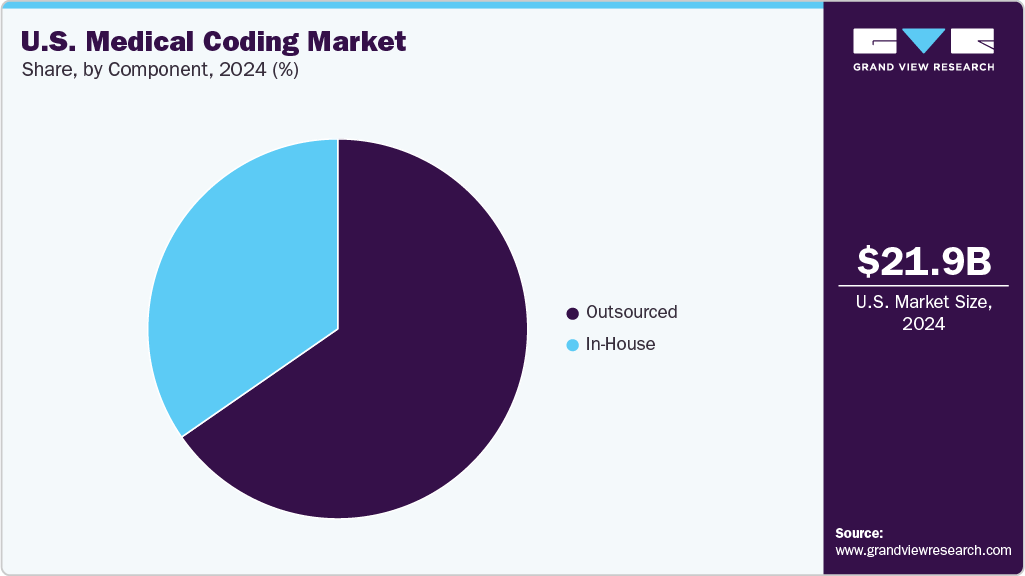
The outsourced segment accounted for the largest revenue share of 64.8% in 2025. Healthcare providers are increasingly outsourcing their medical coding requirements to reduce administrative costs. Outsourcing helps in cost reduction, saves time, and streamlines workflow. Thus, healthcare providers can focus on quality patient care and patient engagement. Rising in offshoring and onshoring of revenue cycle management along with medical coding are positively impacting the market growth. For instance, in August 2021, GeBBS Healthcare Solutions acquired Aviacode, a Salt Lake City-based medical coding and compliance service provider, to expand its technology-enabled Revenue Cycle Management (RCM) services. This acquisition enhances GeBBS's end-to-end RCM offerings, expands its U.S.-based delivery capabilities, and strengthens its medical coding, audit, and clinical documentation improvement portfolio.
The in-house segment is estimated to grow at a steady CAGR during the forecast period. Through in-house medical billing, coding, and revenue cycle management, healthcare providers can retain control over entire operations. Moreover, in case of errors, in-house coders are easily accessible. However, high cost associated with in-house coding owing to requirement of skilled coders, software, and infrastructure is increasing adoption of outsourcing. Outsourcing component is fastest-growing segment owing to its advantages such as reduction in operating costs, claim denials, and increased scalability.
End Use Insights
The acute care hospitals segment led the U.S. medical coding market, accounting for the largest revenue share of 76.9% in 2025. This segment is a major end-user of medical coding services in the U.S., owing to the high volume and complexity of inpatient and emergency care. Hospitals implement coding audits and clinical documentation improvement programs to strengthen coding accuracy and regulatory compliance. These practices support efficient claims processing, reimbursement optimization, financial sustainability, and healthcare workforce management for acute care providers. For instance, in October 2024, Tanner Health and Healthliant Ventures partnered with Corti to deploy AI for medical coding, reducing administrative workload by 80% and errors by 40%. Such factors are expected to harness segment growth.
Similarly, in November 2025, XpertDox partnered with CHP Berkshires, a Massachusetts FQHC serving 30,000+ residents, to deploy XpertCoding AI across all facilities for enhanced medical coding and revenue cycle performance.
"We've successfully implemented XpertDox's AI, and the results have been transformative. We've seen increased collections per claim, higher quality scores through automated Category II coding, and our coding team is now able to focus on value-based care initiatives and auditing. The dashboards for provider documentation improvement and HCC recapture have been especially impactful. The XpertDox team has been great to work with."
-Jesse Suphan, Senior Director of Revenue Cycle & Quality at CHP Berkshires.
The Ambulatory Surgery Centers (ASC) segment is projected to grow at the fastest CAGR during the forecast period, driven by the shift from inpatient to outpatient surgical procedures. Advances in minimally invasive techniques, anesthesia, and post-operative care enable more procedures to be safely performed in ASCs. Specialties including orthopedics, ophthalmology, gastroenterology, and pain management increasingly rely on ASCs for same-day surgeries. As surgical volumes rise, the need for precise coding of procedures, anesthesia services, and diagnostic documentation increases, expanding the role of medical coding in ASC revenue cycle operations.
Key U.S. Medical Coding Company Insights
The U.S. medical coding market landscape is fragmented, with the presence of several small companies holding majority stake. New expansion activities, product approvals, product launches, partnerships, and acquisitions have positively impacted the U.S. medical coding industry in recent years.
Key U.S. Medical Coding Companies:
- Oracle
- Maxim Healthcare Services (Amergis)
- Datavant
- Aviacode Inc (GeBBS)
- Precyse Coding Solutions, LLC
- Verisk Analytics, Inc.
- Omega Healthcare Management Services
- PrimEra Medical Technologies
- Dolbey
- 20/20 MD
Recent Developments
-
In February 2026, Qventus launched the Care Gap and Coding Automation Suite, an AI-driven solution designed to identify missed diagnoses, trigger timely clinical interventions, and automate real-time documentation within provider EHR workflows. By reducing manual administrative burden and improving documentation accuracy to better reflect care complexity, the launch is expected to accelerate adoption of AI-enabled coding and revenue cycle automation tools, thereby supporting growth in the medical coding market.
-
In November 2025, Netsmart launched AlphaCoding, an augmented intelligence solution designed to enhance clinical coding accuracy, efficiency, and compliance across post-acute and human services settings. Built on advanced AI models and aligned with CMS standards, the platform provides near real-time, evidence-based coding recommendations to healthcare professionals. The introduction of AI-driven coding tools is expected to accelerate automation adoption, improve reimbursement accuracy, and stimulate growth in the medical coding technology market.
-
In August 2025, Infinx partnered with Maverick AI to introduce instant autonomous medical coding for revenue cycle management. This strategic collaboration combines Maverick’s advanced AI-powered coding agents with Infinx’s AI-driven revenue cycle platform, enabling real-time clinical summarization, autonomous code assignment, and scalable workflow automation.
“Medical coding undoubtedly remains one of the significant challenges within today’s revenue cycle landscape. The solution devised by Maverick’s team is exceptional-AI that comprehends clinical context and delivers outcomes with unparalleled speed and precision.” -Jaideep Tandon, CEO of Infinx.
-
In October 2024, Corti partnered with Tanner Health and Healthliant Ventures to accelerate medical coding, reducing administrative workload by 80% and improving billing accuracy.
-
In April 2024, GeBBS Healthcare Solutions, Inc. acquired CCD Health, a Dominican Republic based provider of Patient Experience Services. This strategic expansion strengthens GeBBS’ global delivery capabilities and enhances its end-to-end RCM portfolio, supporting market growth through broader service integration, nearshore scalability, and improved patient engagement solutions for healthcare providers and payers.
-
In January 2023, AQuity expanded their coding solutions portfolio with the launch of QCode AI Autonomous Coding.
U.S. Medical Coding Market Report Scope
Report Attribute
Details
Market size value in 2026
USD 23.4 billion
Revenue forecast in 2033
USD 44.4 billion
Growth rate
CAGR of 9.6% from 2026 to 2033
Base year for estimation
2025
Historical data
2021 - 2025
Forecast period
2026 - 2033
Quantitative units
Revenue in USD million/billion CAGR from 2026 to 2033
Report coverage
Revenue forecast, company ranking, competitive landscape, growth factors, trends
Segments covered
Classification system, component, medical specialty, end use
Country scope
U.S.
Key companies profiled
Oracle; Maxim Healthcare Services (Amergis); Datavant; Aviacode Inc (GeBBS); Precyse Coding Solutions, LLC; Verisk Analytics, Inc.; Omega Healthcare Management Services; PrimEra Medical Technologies; Dolbey; 20/20 MD
Customization scope
Free report customization (equivalent up to 8 analysts working days) with purchase. Addition or alteration to country, regional & segment scope.
Pricing and purchase options
Avail customized purchase options to meet your exact research needs. Explore purchase options
U.S. Medical Coding Market Report Segmentation
This report forecasts revenue growth at the country level and provides an analysis of latest industry trends in each of the sub-segments from 2021 to 2033. For this study, Grand View Research, Inc. has segmented the U.S. medical coding market report based on classification system, component, medical specialty, and end use:
-
Classification System Outlook (Revenue, USD Million, 2021 - 2033)
-
ICD
-
HCPCS
-
CPT
-
-
Component Outlook (Revenue, USD Million, 2021 - 2033)
-
In-house
-
Outsourced
-
Onshore
-
Offshore
-
-
-
Medical Specialty Outlook (Revenue, USD Million, 2021 - 2033)
-
Oncology
-
Cardiology
-
Anesthesia
-
Radiology
-
Pathology
-
Pain Management
-
Emergency Services
-
Others
-
-
End Use Outlook (Revenue, USD Million, 2021 - 2033)
-
Acute Care Hospitals
-
Inpatient Settings
-
Outpatient Settings
-
-
Ambulatory Surgery Centers (ASC)
-
Frequently Asked Questions About This Report
b. The U.S. medical coding market size was estimated at USD 21.6 billion in 2025 and is expected to reach USD 23.4 billion in 2026.
b. The U.S. medical coding market is expected to grow at a compound annual growth rate of 9.6% from 2026 to 2033 to reach USD 44.4 billion by 2033.
b. ICD dominated the U.S. medical coding market with a share of over 69% in 2025.
b. Some key players operating in the U.S. medical coding market include Oracle; Maxim Healthcare Services (Amergis); Datavant; Aviacode Inc (GeBBS); Precyse Coding Solutions, LLC; Verisk Analytics, Inc.; Omega Healthcare Management Services; PrimEra Medical Technologies; Dolbey; 20/20 MD.
b. Errors in billings, insurance fraud, and misinterpretations of medical documents result in large financial losses. Increasing losses due to ineffective medical billing and revenue cycle management are increasing demand for revenue cycle management including medical coding software and services. This, in turn, is estimated to drive market growth potential.
Share this report with your colleague or friend.
Need a Tailored Report?
Customize this report to your needs — add regions, segments, or data points, with 20% free customization.

ISO 9001:2015 & 27001:2022 Certified
We are GDPR and CCPA compliant! Your transaction & personal information is safe and secure. For more details, please read our privacy policy.
Trusted market insights - try a free sample
See how our reports are structured and why industry leaders rely on Grand View Research. Get a free sample or ask us to tailor this report to your needs.